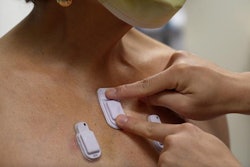
The use of wearable activity trackers to improve physical activity in hospitalized adults was recently investigated in a systematic review and meta-analysis.
The results, published Thursday in JAMA Network Open, associated the trackers with higher physical activity levels, less sedentary behavior, and better physical functioning when compared with usual care outcomes.
Hospitalization is generally characterized by very low levels of patient physical activity. These low activity levels may contribute to a range of poor patient outcomes, including increased mortality, functional decline, frailty, and disability. Conversely, observational studies show that higher physical activity levels during hospitalization are associated with shorter lengths of stay and reduced readmission rates. Even small in-hospital activity levels of just 900 steps per day appear to prevent subsequent functional decline.
Efforts to improve patient physical activity during hospitalization are growing. Interventions using wearable activity trackers are gaining popularity in hospitalized populations for their ability to promote physical activity using behavior change techniques, including self-monitoring, goal setting, and feedback. However, the association between the trackers and hospital efficiency outcomes, as well as clinical outcomes including physical function, are not completely understood.
The researchers sought to evaluate the association between interventions using wearable activity trackers during hospitalization and patient physical activity, sedentary behavior, clinical outcomes, and hospital efficiency outcomes.
Fifteen studies with 1,911 total participants were included in the meta-analyses. These represented four studies of various surgical cohorts, three of stroke rehabilitation, three of orthopedic rehabilitation, three of mixed rehabilitation, and two mixed medical studies. Primary outcomes were objectively measured physical activity or sedentary behavior. Secondary outcomes included clinical outcomes such as physical function, pain, and mental health, as well as hospital efficiency outcomes including length of stay and readmission.
Significant associations were found between wearable activity tracker interventions and higher overall physical activity and less sedentary behavior. Significant associations were also found between wearable activity tracker interventions and improvements in physical function, compared with usual care. No significant associations were found between wearable activity tracker interventions and pain, mental health, length of hospital stay, or readmission risk.
The indications that wearable activity trackers can increase patient physical activity, reduce sedentary behavior, and enhance physical function during hospitalization may make these trackers a useful tool for supporting patient recovery.
“This systematic review and meta-analysis found that using wearable activity trackers during hospitalization is associated with higher patient physical activity and less sedentary behavior, along with modest improvements in physical function,” the authors concluded in their paper. “Although no association was observed with hospital efficiency outcomes, the growing body of evidence suggests that wearable activity trackers hold promise for improving patient activity and supporting recovery during hospitalization. As healthcare becomes increasingly digitized, further exploration of the clinical outcomes and cost-effectiveness of wearable activity trackers in different groups who are hospitalized will be crucial for guiding their use and maximizing their potential benefits.”