A test that incorporates the analysis of genetic mutations in pancreatic cyst fluid and artificial intelligence (AI) algorithms is helpful for making the call on benign findings, with potential to spare patients from unnecessary surgeries, researchers reported in Science Translational Medicine on July 17.
The test -- dubbed comprehensive cyst, or CompCyst -- incorporates mutation status, loss of heterozygosity, aneuploidy, protein markers, and clinical data. An artificial intelligence algorithm is used to help identify which patients should have surgery and which ones can be followed safely.
In a retrospective, multicenter study of 862 patients with pancreatic cysts who had surgery, the test added useful information beyond what is used to manage patients in standard care -- that is, clinical features, nonspecific fluid tests, and imaging studies -- for determining if cysts were benign or malignant, reported Dr. Bert Vogelstein, co-director of the Ludwig Center at Johns Hopkins Kimmel Cancer Center, and colleagues in Science Translational Medicine.
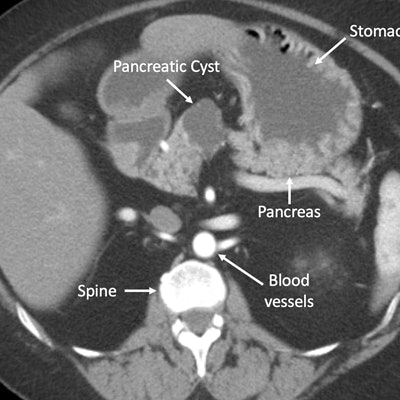
 Computed tomography (CT) image of the pancreas with a cyst. Image courtesy of Johns Hopkins Kimmel Cancer Center.
Computed tomography (CT) image of the pancreas with a cyst. Image courtesy of Johns Hopkins Kimmel Cancer Center.Standard methods for characterizing cysts identified 19% of patients with a benign cyst, whereas adding CompCyst resulted in the correct identification of 60%. For those with mucin-producing types of cysts and no dysplasia or invasive cancer, standard clinical management identified 34% of benign cysts, compared with 49% for CompCyst.
"We calculated that relative to the current clinical practice, CompCyst would have decreased the number of operations done for benign nonmucin-producing cysts, which in hindsight were unnecessary, by 74%," Dr. Marco Dal Molin, a postdoctoral research fellow at the Johns Hopkins Kimmel Cancer Center, said during a press briefing on July 16. "Overall, the use of CompCyst would have avoided unnecessary surgery in 60% of the patients included in this study."
Current criteria are sensitive but not very specific, resulting in a relatively high rate of nontherapeutic operations, Dal Molin said.
"Our study directly addresses these limitations and has the potential to be a major leap forward in the management of pancreatic cysts," Dr. Christopher Wolfgang, PhD, director of hepatobiliary and pancreatic surgery at the cancer center, said during the briefing. "If these results translate into clinical practice, a large number of patients will be spared an unnecessary operation with associated mortality and lifelong morbidity."
"And, importantly, there will be no sacrifice in the ability to identify cancers or worrisome precursor lesions such as high-grade dysplasia," Wolfgang added.
The researchers hope the test will become available at Johns Hopkins within six to 12 months and that a prospective study will be done to pave the way for approval by the U.S. Food and Drug Administration. A newly launched company called Thrive Earlier Detection has licensed rights from Johns Hopkins.
Addressing a clinical conundrum
Pancreatic cysts are estimated to be present in 4% of people in their 60s and 8% of people in their 70s, and they are commonly seen on imaging studies.
"The fundamental problem with cysts is that the vast majority of these cysts are completely benign and will never progress to cancer," Wolfgang said. "This even includes the mucinous neoplasms which are precancerous."
Operations have an associated mortality rate of 1% to 3%, entail a long recuperation period, and may have a lifelong effect on quality of life, Wolfgang said. Consequently, he added, surgery "must be reserved for only those who would truly benefit" -- those few patients whose cysts would develop into cancer, which has a high mortality rate. However, in practice, 25% of cysts turn out to be benign upon surgical resection, and up to 78% of mucin-producing cysts identified through surgery are not advanced, the researchers noted in their write-up.
For the study, three molecular tests were performed -- to evaluate gene mutations, losses in genes, and aneuploidy -- as well as a protein panel. The mutation test included 11 genes associated with the growth or suppression of cells in pancreatic cancers. Dal Molin explained during the briefing that the goal was not to replace current practice incorporating clinical data and imaging characteristics but "rather to integrate all of these aspects together." All of the information was then analyzed with the Multivariate Organization of Combinatorial Alterations (MOCA) machine-learning algorithm.
"The MOCA algorithm tests millions of combinations of features to identify markers that predict the correct treatment pathway with the highest sensitivity and specificity," Dal Molin said. "Because of the large number of patients included in the study, we were able to train our algorithm in half of the patients and to validate it in a completely independent core represented by the second half of the patients."
The researchers assessed retrospectively whether cysts did not need monitoring, required periodic monitoring, or posed a high risk and should be surgically resected. Test results were compared with histopathological analysis of resected surgical specimens.
A closer look at mutations
Among other findings, the investigators reported that 59% of serous cystic neoplasms -- the most common type of benign cyst -- had mutations in the VHL gene or heterozygosity in the chromosome where the VHL gene is located.
"[Vascular endothelial growth factor A (VEGF-A)] has previously been reported as a promising marker for identifying serous cysts, the commonest type of benign pancreatic cyst," the group wrote in Science Translational Medicine. "In our study, elevated VEGF-A concentrations were found in serous cystic neoplasms, as well as some mucin-producing cysts and malignant cysts.
Looking at mucin-producing cysts, the researchers also found more mutations in 76% of intraductal papillary mucinous neoplasms (IPMNs) versus 43% of mucinous cystic neoplasms (MCNs).
"GNAS mutations were highly specific for mucin-producing cysts and were not identified in any other cyst type," the authors wrote. "In contrast, KRAS mutations were found in a number of other types of pancreatic cysts including 3% of benign cysts and 85% of pancreatic adenocarcinomas."
Using a threshold of 192 ng/mL in carcinoembryonic antigen (CEA) cyst fluid tests, the sensitivity of CEA for differentiating mucin-producing cysts is 38% and the specificity is 96%, they wrote.
The cases reported represent just a fraction of the number of patients with pancreatic cysts from Johns Hopkins and collaborating institutions -- not a representative sample of all patients, the researchers acknowledged.
"In future years, when more data becomes available, we hope that the same paradigm and the same algorithms can be used to further improve the results and performance," Vogelstein said.