An antibody blood test has been validated for an increasingly common and troublesome type of malaria, an international team reported in Nature Medicine on May 11. A similar approach is now being explored in COVID-19, with potential for the development of a better antibody diagnostic for community surveillance, investigators suggested.
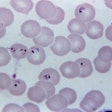
In the article, investigators shared their experience with the development and evaluation of a panel of serological markers to measure antibody responses to liver-stage parasites, or hypnozoites, which are found in people with malaria caused by Plasmodium vivax. This type of malaria is known to lie dormant, noted an international research team from the Walter and Eliza Hall Institute of Medical Research in Australia, the Pasteur Institute in France, and Ehime University in Japan.
The researchers set out to develop a test that would classify the infection based on a range of immunoglobulin G (IgG) antibody responses to P. vivax.
 A new blood test has been validated for P. vivax malaria and researchers believe something similar could work for COVID-19. Courtesy of Mayeta Clark, Walter and Eliza Hall Institute.
A new blood test has been validated for P. vivax malaria and researchers believe something similar could work for COVID-19. Courtesy of Mayeta Clark, Walter and Eliza Hall Institute."These hypnozoites, undetectable with current diagnostics, can be responsible for >80% of all blood-stage infections," wrote co-lead author Dr. Rhea Longley, a researcher at the Walter and Eliza Hall Institute, and colleagues. "Identifying and targeting individuals with hypnozoites is thus essential for accelerating and achieving malaria elimination."
To develop the blood test for serological markers, researchers screened 342 P. vivax proteins and decided on a panel of eight. In samples taken from areas where malaria is endemic -- parts of Thailand, Brazil, and the Solomon Islands -- the test had 80% sensitivity and specificity for classifying P. Vivax, the team reported. The results suggest that the panel test is an effective method for indirectly identifying likely carriers of liver parasites associated with infection.
"These eight antibody responses can serve as a biomarker, identifying individuals who should be targeted with anti-hypnozoite therapy," the authors wrote.
Targeting a public health barrier
Malaria caused by P. vivax has presented a barrier to the public health goal of eliminating malaria in countries where the disease is endemic by 2030, the authors noted. Mathematical modeling studies show that serological testing and treatment could reduce P. vivax prevalence by 59% to 69%.
"A major hurdle for elimination is the increasing proportion of malaria cases caused by P. vivax as malaria endemicity declines," Longley and colleagues explained. "P. vivax has unique biological features that make its control difficult, including high prevalence of low-density, asymptomatic infections and a liver stage that can reactivate weeks to months after initial infection, resulting in relapses that cause morbidity and [sustained] transmission."
Researchers are working with Australian biotech company Axxin to develop a commercial diagnostic test for field use in Malaria-stricken countries based on the biomarkers that have been identified. They are also exploring application of a similar approach for detection of antibodies in people who have been infected with the novel coronavirus, SARS-CoV-2.
"Many tests for immunity give a simple 'yes or no' answer to whether someone has antibodies to the infectious agent," said research leader Ivo Mueller, PhD, of the Pasteur Institute and also the Walter and Eliza Hall Institute.
"In contrast, our test -- which was initially developed to look at malaria infections -- can pinpoint how long ago a person was exposed to an infection," he said in a statement about the malaria data.
This information is useful for community surveillance, the researchers said. Mueller and colleagues published experience with serological signatures of SARS-CoV-2 and implications for antibody diagnostics in a preprint submitted on May 11 to Hyper Articles en Ligne (HAL), an open archive for scholarly documents.