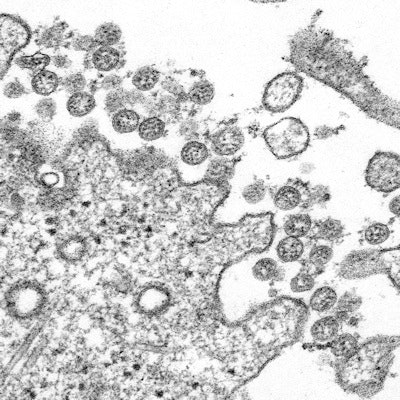
The continued spread of the novel 2019 coronavirus, known as SARS-CoV-2, around the world has raised the need for a test to rapidly and efficiently screen coronaviruses to monitor rapid changes and determine how they function. Findings from ongoing U.S. National Institutes of Health (NIH) research, published in Nature Microbiology on February 24, offer new tools in the fight.
The rise of next-generation sequencing has led to a boom of viral sequence discovery. The genus betacoronavirus is divided into four lineages (A-D) and contains a number of human viruses. Lineage B has around 200 published virus sequences and includes the severe acute respiratory syndrome coronavirus (SARS-CoV) and the newly emerging SARS-CoV-2 (previously called 2019-nCoV). It is still unknown if other viruses in this lineage have the potential to emerge in humans. Moreover, current techniques to study whether these viruses can enter human cells are technically demanding, time-consuming, and expensive.
Many viruses, including betacoronaviruses, use cell entry as a means of cross-species transmission. All coronaviruses encode a surface glycoprotein -- a spike -- that binds to the host-cell receptor and mediates viral entry. The host receptor for SARS-CoV-2 has been identified as angiotensin-converting enzyme 2 (ACE2). For betacoronaviruses, a single region on the spike called the receptor-binding domain (RBD) mediates this binding interaction. After binding, the host proteases cleave the spike, facilitating virus entry.
With underlying mechanisms in mind, and with the goal of overcoming testing limitations, Michael Letko, PhD, and colleagues from the NIH took a reductionist approach to studying coronavirus entry. They developed a scalable, biosafety level 2-compatible method for detecting the minimal region of coronavirus that's essential for interacting with a host receptor.
Relying on the principle that RBDs on coronavirus spikes are capable of folding independent of the rest of the spike protein, and that they contain all of the information needed for host receptor binding, the NIH researchers tested receptor usage of all published unique RBD sequences for lineage B coronaviruses.
They found that lineage B RBDs divide into three functionally distinct clades. Only clade 1 RBDs contain all 14 residues that have been shown through crystallography to interact with human ACE2. Using synthetic biology and molecular engineering, combinations of coronaviruses were generated to test the specificity of RBDs, the importance of protease in viral entry, and whether these two processes are coupled.
The studies revealed that protease-mediated entry is receptor dependent, with ACE2 entry being lineage B clade 1 specific. However, when the spike was genetically modified in clade 2 and 3 viruses, viral entry was improved to varying degrees. This suggests that the limiting factor of viral transmission may be protease processing.
Interestingly, the RBD for SARS-CoV-2 has residues and motifs found in all three clades but uses ACE2. This may explain the human-to-human transmissibility of the virus. It contains most of the contact points with human ACE2 that are found in clade 1 and some amino acid variations that are unique to clades 2 and 3. The researchers suggest that it may be possible that SARS-CoV-2 arose from recombination between clade 1 and the other clades.
Overall, the results of the study emphasize the importance of continued surveillance of coronaviruses at the sequence and functional levels in order to better prepare for the next emerging virus.



















