Testing patients with high-risk bowel cancer symptoms twice in succession improves disease detection, a clinical trial has found.
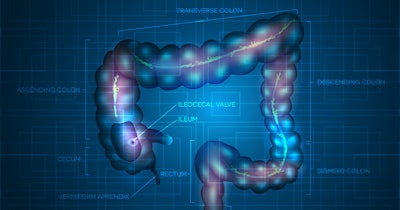
The fecal immunochemical test (FIT), which looks for blood in stool samples, is commonly used as part of the investigation of people who have symptoms of colorectal cancer. If the FIT comes back positive, the patient is sent for further investigation that will determine if the blood found in their stool is the result of a tumor.
However, the test can deliver false negatives that may delay further investigation and the diagnosis and treatment of colorectal cancer. FIT has a sensitivity of 87% at 10 µg hemoglobin per gram of feces. To try to raise the sensitivity, researchers at the University of Edinburgh explored the effects of testing twice.
The study, details of which were published in the British Journal of Surgery, suggests that there may be value to performing two FITs in succession. The researchers assigned symptomatic patients to two cohorts. In the first cohort, 2,260 patients completed one FIT and investigation. In the second cohort, 2,637 patients completed two FITs and investigation. Patients in the second cohort were sent two FITs 13 days apart, on average. All subjects were investigated, regardless of the FIT result.
Single-FIT had a sensitivity of 84.1% for colorectal cancer and 67.4% for significant bowel pathology. In the double-FIT cohort, the sensitivities for colorectal cancer and significant bowel pathology were 96.6% and 83%, respectively. As such, the second FIT reduced the number of missed cancers by 50% and the number of missed significant bowel pathologies by 30%.
Study co-author Farhat Din, reader at the University of Edinburgh and consultant surgeon at Western General Hospital in the same city, discussed the findings and the real-world implementation of the two-test approach.
“Our study highlights how to maximize use of FIT in symptomatic patients. Use of two FIT tests will miss less bowel cancer with a positive impact on patient care. Locally, implementation of the double-FIT strategy has led to a reduction in endoscopy without adversely affecting cancer detection rates,” Din said in a statement.
The authors note some limitations of the study, however. Cohort one completed enrollment before cohort two began enrollment. The second cohort, which began in March 2020, was affected by the pandemic and the researchers warn that “direct comparisons between the single-FIT and double-FIT cohorts are challenging because of inherent differences created by the two time intervals.”