Researchers from Switzerland and Washington University in St. Louis are developing new SARS-CoV-2 virus testing techniques to add to the current toolkit for diagnosis, which currently revolves around reverse transcription polymerase chain reaction (RT-PCR) technology.
The findings of the two studies -- one published on April 13 in ACS Nano and the other on April 20 in Nature Biomedical Engineering -- could offer clinicians more ways to quickly diagnose the presence of the virus, which is key to controlling its spread.
And although RT-PCR assays tend to be accurate, in some countries test kits have been in limited supply or results have piled up in a backlog. Furthermore, the RT-PCR test isn't perfect, wrote a team led by Dr. Guangyu Qiu of the Institute of Environmental Engineering in Zürich.
"Reliable laboratory diagnosis of the disease has been one of the foremost priorities for promoting public health interventions," Qiu and colleagues wrote.
RT-PCR is a routinely used reference method for the diagnosis of COVID-19, but there have been several reports of false positive or negative cases, especially in the early stages of the outbreak of the novel coronavirus, they noted.
Signs of strain
Millions of patients have been tested for SARS-CoV-2 with RT-PCR kits, the American Chemical Society (ACS) said in a statement released with the Qiu et al study.
"This sensitive method amplifies SARS-CoV-2 RNA from patient swabs so that tiny amounts of the virus can be detected," the ACS said. "However, as the pandemic surges, this laboratory workhorse is showing signs of strain."
In response, Qiu and colleagues sought to develop a fast, accurate assay for identifying the SARS-CoV-2 virus as an alternative to RT-PCR testing. The test they developed is based on a technique called localized surface plasmon resonance, which detects interactions between molecules, according to the ACS.
"The team made DNA probes that recognized specific SARS-CoV-2 RNA sequences and attached them to gold nanoparticles," the ACS said. "When they added pieces of the virus's genome, the RNA attached to the complementary probes like a zipper being closed. The team used a laser to heat up the nanoparticles, making it more difficult for imperfectly matched sequences to remain attached, reducing false-positives."
This "zipper" quality was able to help the researchers discriminate between SARS-CoV-2 and SARS-CoV-1, its close cousin. Furthermore, the test could detect viral RNA in concentrations as low as 0.22 pM -- lower than those found in respiratory swabs, the group noted.
The new assay needs to be tested on intact viral RNA from patient samples, according to Qiu and colleagues. But it's a promising technique.
"Under the outbreak background of COVID-19, this proposed [technique] can provide a reliable and easy-to-implement diagnosis platform to improve the diagnostic accuracy in clinical tests and relieve the pressure on PCR-based tests," the group concluded.
Turn up the light
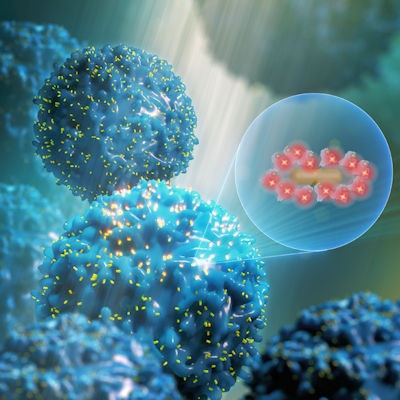
In the second study, researchers from the McKelvey School of Engineering at Washington University in St. Louis described a rapid SARS-CoV-2 test they are developing that uses an ultrabright fluorescent nanoprobe called plasmonic fluor. The test will be 100 times more sensitive than the RT-PCR assay, which could reduce false negatives, according to the team led by Srikanth Singamaneni, PhD.
 Engineers at the McKelvey School of Engineering have received federal funding to develop a rapid COVID-19 test using a newly developed technology called plasmonic fluor. Image courtesy of Washington University in St. Louis.
Engineers at the McKelvey School of Engineering have received federal funding to develop a rapid COVID-19 test using a newly developed technology called plasmonic fluor. Image courtesy of Washington University in St. Louis.In biomedical research and clinical applications, fluorescence is a useful way to target molecules. But at times it's not strong enough, according to Singamaneni.
"The problem in fluorescence is, in a lot of cases, it's not sufficiently intense," he said in a statement released by the university. "If the fluorescent signal isn't strong enough to stand out against background signals, just like fireflies against the glare of the sun, researchers may miss seeing something less abundant but important."
The new technology is composed of gold nanoparticles coated with dyes that "turn up the brightness" of fluorescent labels, the university said. These nanolabels act as "an ultrabright flashlight," identifying small amounts of molecules such as SARS-CoV-2.
Singamaneni's team has received federal funding to further develop the technology.